by Hana Tisserand
 The beautiful French town of Grasse has a long and scented history. It has been dubbed the world capital of fragrance, and in the 19th century its abundant flower fields, now mostly replaced by villas, gave rise to a still-thriving perfume industry. In Grasse, fragrance brands and stores are ubiquitous, and there are even several fragrance museums. Some of the local specialties are fragrant, like fougassette – an orange blossom infused bread, which is delicious!
The beautiful French town of Grasse has a long and scented history. It has been dubbed the world capital of fragrance, and in the 19th century its abundant flower fields, now mostly replaced by villas, gave rise to a still-thriving perfume industry. In Grasse, fragrance brands and stores are ubiquitous, and there are even several fragrance museums. Some of the local specialties are fragrant, like fougassette – an orange blossom infused bread, which is delicious!
On October 6th and 7th 2017, the town hosted the 18th Phyt’Arom conference, which is dedicated to aromatherapy and phytotherapy. This year’s topic was Phytotherapy & Aromatherapy in Medical and Hospital Care. (In France, aromatherapy is very often combined with phytotherapy, or herbal medicine.) Twenty-two speakers shared the stage for two days of lectures and workshops, and Robert Tisserand and I attended. Read on to find what we learned about French aromatherapy in hospitals, how safety is tackled, how tradition is combined with research, what can be done for the caregivers, and what the situation is with essential oils in pharmacies.
Aromatherapy à la Française
Many consider France the cradle of modern aromatherapy – after all, it was largely through the works of René Maurice Gattefossé, Dr Jean Valnet and Marguerite Maury, that essential oils started to reclaim their rightful place in healing and medicine in the 20th century. And Grasse, in turn, is where modern perfumery was born and where it, quite literally, flourishes to the present day. When we toured the International Museum of Perfume in Grasse, our guide introduced us to the three historical functions of fragrance – prayer, seduction, and healing. And what is aromatherapy if not healing with natural fragrance?
The museum is to die for – the website does not do it justice. We were dazzled by the thousands of fragrant containers and bottles from ancient to modern. These included an impressive number of ancient Egyptian, Greek and Roman flasks. We were equally enchanted by the gardens of aromatic plants, which included Patchouli, Vetiver, Cistus, Ginger (which was in flower and smelled amazing!), Mimosa, Lemon Verbena, Geranium, Jasmine Sambac, Cassis, Sage, Myrtle, Melissa, Vanilla, and many others, including mature Orange trees. To illustrate the various types of extraction there were models, photographs and equipment to illustrate distillation, enfleurage etc. The history of perfumes in Grasse was of course well represented.

Ginger in bloom
There are some assumptions about French aromatherapy. The so-called “French school” is usually linked to the use of large amounts of essential oils, often via ingestion. And since we always like to go to the source for any information, we went to France to find out if the reality of French aromatherapy resembles the perception. And what better opportunity to do so than a conference that showcases the latest developments? This year’s program promised many inspiring talks on topics ranging from urinary tract infections to using aromatherapy in helping the helpers.
Robert and I were really looking forward to learn more about the French approach. What we totally did not expect was to find that they are doing almost exactly what we have been advocating for, and that aromatherapy in France is changing. We listened to speaker after speaker talking about proper dilution, the importance of safety. Some even advocated for the preference of topical application and inhalation over ingestion. This, it has to be said, was in the context of the need for aromatherapy to be accepted as a viable modality in French hospitals, but it was still a surprise. Rhiannon Lewis, who helped organize the conference, explained privately that this current trend only started a few years ago. Robert commented that “the French are discovering essential oil safety!” Not entirely true, but this did very much encapsulate the current mood.
Into the hospital – with proof of safety and efficacy
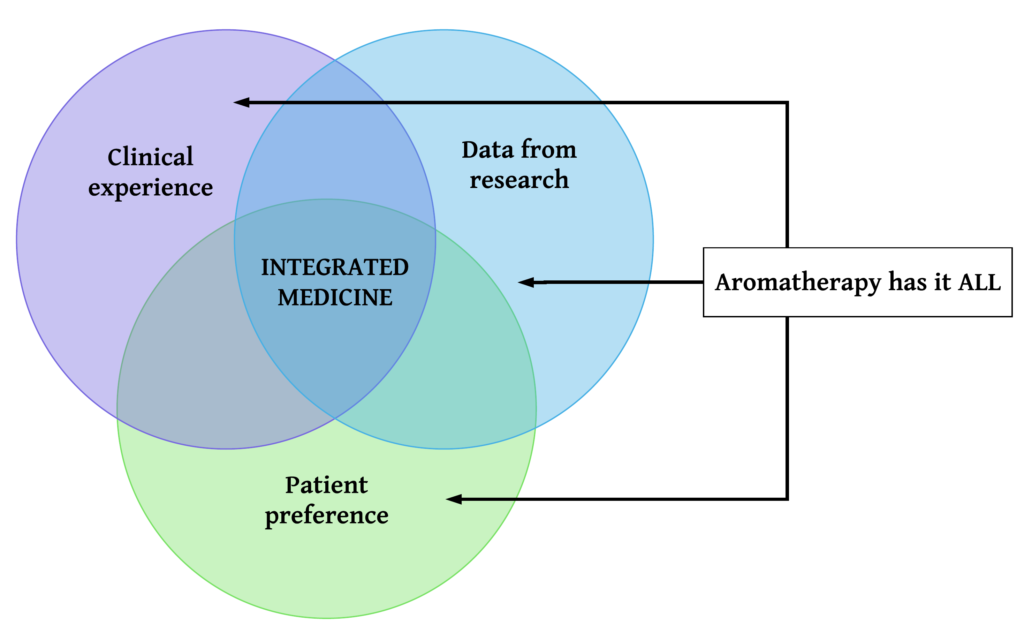
If there was an underlying theme for the whole event, it was the call for a truly integrated medicine. As we have seen again and again, both in practice and in clinical studies, essential oils are proving to be incredibly useful in hospital settings, and it is this aspect of aromatherapy that the French are trying to harness. Jacques Kopferschmitt, who delivered the opening presentation, stressed that for a modality to be used in a state-wide healthcare system, it needs to be accepted by the administrators. And for this to happen, research-based evidence of both therapeutic efficacy and safety is needed. Any such modality, in our case the use of essential oils, also has to be both financially viable and practical.
Professor Kopferschmitt pointed out that a truly integrative medicine combines clinical experience with scientific data, while also taking into account the preferences and needs of the individuals treated. And quite optimistically, he stated that the use of essential oils is in “pole position” among other alternative medicine modalities, as it has all three elements. Nevertheless he called for a more robust body of research to show that aromatherapy can justify its place in modern medicine. And the French are trying to assert that place very firmly.
A 200 page white paper called, in translation, The Consensus of Experts Guiding Education, Practice and Scientific Assessment of Aromatherapy in the Hospital Environment, is due to be published in January 2018. Since 2014, an expert panel consisting of doctors, nurses, pharmacists and aromatherapists, has been assembling a comprehensive set of guidelines for the integration of aromatherapy into hospital care in France. As far as we know, this is the first centralized attempt to make aromatherapy an accepted modality in hospitals on a national level. The current status of the work was presented at the conference, by a group consisting of Dr Geraldine Gommez, Dr Michel Faucon, Emmanuelle Guillemin, a senior health manager, and Isabelle El Khiari, a clinical nurse. Their publication tackles all the areas that need to be evaluated before an aromatherapy protocol can be introduced into a medical facility – from education structure, to financial rationale, to safety. And that is where we were most surprised!
Moderation at the forefront
For years, aromatherapy in France has indeed centered on both ingestion, and on the use of high concentrations of essential oils on the skin. What we heard during the presentation of Scientific Aromatherapy (the working group for the Consensus) was an emphasis on inhalation, and dilutions of 10% or less – at times even more conservative than the guidelines in Essential Oil Safety, 2e. Dr Faucon, known for his robust book Traité d’Aromatherapie Scientifique et Médicale, spoke very clearly against using undiluted essential oils topically. He advocated for intermittent diffusion in the hospital environment, as distinct from continuous diffusion. He added that diffusers should not involve the use of water (to eliminate the risk of bacterial growth) that they should not contain any glass parts (because of the risk of breakage) and that none should involve a naked flame. All of this for safety reasons. As Dr Kopferschmitt stated in his presentation – any use of essential oils needs to be rational, validated and safe.

One of the safety-focused slides by Dr Michel Faucon, cautioning against using undiluted essential oils on the skin, and recommending dilutions of 10% or less
Safety was a topic also featured in a well-balanced presentation by Dr Christine Kopferschmitt, who looked at how using a “sanitizing hope spray” containing 41 essential oils may exacerbate asthma symptoms in people who are asthmatic already, and that it might possibly increase the risk of developing asthma. Safety guidelines should always be based on a carefully measured approach, in order to minimize risks while still maintaining the benefits of aromatherapy. It is perhaps safe to say that no aromatherapist would recommend a blend of 41 oils, but this product has been marketed to consumers in Europe, and the risks linked to its usage should not be ignored.
A novel approach to safety assessment was presented at the conference by Nicolas Dornic. He and his team conducted a survey of 1,500 people, focusing on patterns of topical use of essential oils. The survey revealed the most popular essential oils (Lavender for women, Eucalyptus for men), as well as real-life usage and exposure patterns. And that is where Dornic and his colleagues look for in assessing risk. Instead of the usual deterministic model, they look at the probable exposure, thus being able to calculate the potential risk more accurately. The model is still in development, and will apply to single essential oil constituents as it relies on available toxicology data, however it is a step towards safety guidelines that reflect reality and we will for sure stay in touch with Dornic and his team.
Applied research meets traditional use
Several of the conference presentations were dedicated to new areas of research, and to clinical application of such research, as well as to more traditional uses of essential oils to address various ailments. Dr Auriane Gros presented her group’s research in the management of Alzheimer’s disease through essential oils. This included a novel automated personal diffusion system, based on sophisticated monitoring of a patient’s behavior, and the pulsing out of appropriate essential oil blends as needed by the individual! Results were very promising, but some modifications to the protocol were indicated. Dr Stribor Markovic from Croatia shared his remarks on treating respiratory issues with the help of essential oils, again, combining the latest research with his medical experience from the Balkans, including such specificities as men refusing to take suppositories so as not to appear “gay”.
We were delighted to meet Dr. Jurgen Reichling from the University of Heidelberg, who has made significant contributions to our collective knowledge about essential oils and microbial disease over many years. Dr Reichling talked about the amazing capability of essential oils to penetrate through bacterial biofilms and to subsequently kill bacteria that form them. He also mentioned potential antiviral properties, stressing that essential oils cannot reach viruses that are inside cells, and can only eliminate those that are free-floating or on the surface of a cell, such as the Herpes simplex virus on a cold sore.
Dr Paul Goetz, a phytotherapist from Strasbourg, spoke about treating of urinary tract and vaginal infections. Dr Goetz trained with Paul Belaiche, a contemporary of Jean Valnet, and author of the three-volume work, Traité de Phytothérapie et d’Aromathérapie. Dr Goetz’s approach was a combination of new research discoveries and traditional uses, and in common with the classic French medical aromatherapy model, he routinely combined herbal tinctures with essential oils. His formulations were accompanied by notes on how to tweak the treatment if the patient is exhibiting certain symptoms, stressing the importance of a careful initial consultation as well as continuous monitoring of the patient. As for the doses and dilutions, the oral preparations contained up to 5% of essential oils in alcohol, with doses of essential oil equivalent to 1-2 drops, three times daily. He recommended 1g pessaries for vaginal infections, with 1-4 drops of total essential oil. Even this aromatic medicine protocol seemed conservative in terms of dosage, though most of the time Dr Goetz used herbal preparations.
Aromatherapy helps caregivers too

Perfumer’s costume – a statue in front of the International Museum of Perfume
Both in the UK and in the US aromatherapy has been proving its value in the hospital environment – mainly in palliative care and oncology units. It has a great potential to help with some of the side effects of harsh treatments or chronic conditions, such as pain, itch, nausea, insomnia and anxiety. Now French aromatherapists are harnessing these kinds of properties so that essential oils will be accepted into the broader hospital environment. However, aromatherapy in hospital care can also benefit the staff. From malodor management to the relaxing weekly aromatherapy session, nurses and doctors have benefitted from receiving care, which in turn prevented burnout, so common in caregiving professions. This was the subject of a presentation given by Wendy Belcour and Claire Chauffour-Ader.
We also believe that aromatherapy has an indispensable place in healthcare, and especially where conventional medicine has failed to find viable solutions – chronic conditions, mental health, resistant bacteria… Having essential oils recognized as a safe and effective complementary modality in healthcare facilities is a positive and important step towards it being recognized as a valuable partner in tackling future healthcare challenges. Hearing about the recent developments in France was very encouraging!
How about the pharmacies?
You may have heard that in France, you can buy essential oils in pharmacies, and it is the pharmacists that encourage the use of essential oils. Although not many pharmacists featured among the speakers (the only one being Dr Michel Faucon, who spoke on safety in hospital settings), it was evident that they play a major role in the aromatherapy landscape in France, and one of the session chairs, Dr. Stéphane Pichon, is a well-known pharmacist. As we wanted to learn more about the relationship between pharmacists and aromatherapists, we looked outside the lecture room.
Dr. Guilhem Jocteur is a pharmacist and educator, whose school Apoticarius focuses on educating other pharmacists and medical professionals about essential oils, and teaches them how to conduct an aromatherapy consultation. We approached him at his conference stall to ask how the French really use essential oils. He talked about various gel capsules that are available now (gelules, as they call them), and that those are the preferred method of use for ingestion. When we asked him if putting essential oils in water to drink was an option, his reaction was as swift as surprised: Mais ca ne mélange pas! (But they don’t mix!). He then added that you could use Solubol if you really wanted to take your oils in water, however the taste would still be very strong. H felt that same applied to lactose-based blank tablets that are available in France (comprimées), and that can be used for essential oils. They would still taste too strongly, Dr Jocteur stated. This was at least his take on the approach of pharmacists in France, and he was clearly concerned about both safety and patient compliance, though he added that he could not control what consumers might do at home.
So what is the current status of French aromatherapy?
The event was not without debate, and more than once there was a comment from the audience described as no more than “un petit remarque” which in fact led to lively debate. Dr Reichling, in his presentation, expressed skepticism about the idea that oral dosing of essential oils could possibly be effective in treating infectious disease, since concentrations in blood would be no more than a few nanograms/ml. Others felt that the clinical evidence did in fact support the oral dosing model. Perhaps it depends on the location and virulence of the disease, as well as the exact dosing protocol. At one point it almost looked like a France-Germany conflict, but all ended well, and such debate is vital to the progress of aromatherapy.
During our weekend in Grasse, we learned a lot about how French aromatherapists and medical professionals approach aromatherapy today, and we were indeed surprised to see so much caution and safety awareness, as well as a very firm emphasis on clinical results in the form of published research (usually in English). As for the “French school”, what is actually being taught in French aromatherapy schools is also much more sensible and safety-conscious than we had imagined – we chatted with several educators at the conference. But really, aromatherapy should not be “French”, “British”, “German”, or any other nationality. It should be safe, effective, evidence-based, and appropriate – and we’re getting there. In France, essential oils are certainly perceived as valuable partners to other types of plant medicine as well as, very often, to conventional medicine. We will continue to monitor developments, and there will be more about dosing and “French aromatherapy” in a future post.
The next Phyt’Aroma conference will be held in 2019 – date not yet announced.






Beautiful article, thank you!
This was an awesome article! Thank you so much!
Fabulous! Thankyou for bringing this information to us, maybe one day I can go to France and participate myself just for the emersive experience.
Great read ~ thank you.
Thanks Hana and Robert for keeping us in the loop. I always wondered how much of the so called French School was real or pure marketing tool for some crazies…
Thank you for sharing so vividly and detailed this amazing experience at Grasse Phyt’ Arom!
Great article, beautifully written – thanks Hana!
Enjoyed this very much. Gives credence to my talks about “safety first.”
Thank you Hana for reporting in depth on the trip you and Robert made to the Grasse Conference. Well written and loved the photos. I look forward to more in the future.
Great article, thank you.
Great reading, thank you so much for sharing.
Gracias x compartirlo!!
We are all in awe of the outstanding qualities of the plant kingdom – nature at its best and for once technology has done us proud to succeed in methods that enable us to utilise the benefits of this kingdom – Thank you for your article it certainly helps to inspire us even further. Michelle Australia
Great read and well written. Thank you for sharing with us.
Thank you so much for sharing
Excellent!
Thank you! This was very interesting and educational.
Very interesting article : thank you. I’m a French Pharmacist but I live in the US and I’m now a certified aromatherapist. At first I was using the oils like I’ve read in France. With the certification course and after I have read your book, I started to use it more carefully. That is great that someone like Faucon changes his mind but the problem is that the population is still following some other people who still recommend oil not diluted on the skin. My mom can no longer apply lavender on her skin : she is strongly allergic now as she was not before.
How wonderfully interesting, thank you both so much. There is a heart wrenching tussle here for me – heart, mind & soul. And it seems we are at a bit of a point in time where we are finding the political reality of being drawn to play by the rules of the pharmaceutical medical industrial complex & their rules with having to “prove” people’s stories & experiences are true….. A ffine balance to find indeed, for each of us & collectively. Cheers & best wishes to each & every one of us in this! May you find beauty in each day x
Great update on French aromatherapy. Will re-write my notes 😊 Thank you, Hanko!
Thanks for sharing such an interesting information.
Very good article! Thank you!
Hana, thank you so much for a thorough reporting of this event and what you and Robert learned. You keep the rest of us up to date on these issues that are important in the field of aromatherapy.
Great read!!
Wonderful! And so promising! Thank you for sharing Hana!
Fabulous article!
Thanks a lot Interesting report, just remember therapeutic use with oral intake of essential oils is described in middle” of 19 th century : Swain syrup including wintergreen oil against Syphilis.We can even find french formula books(1775) including Anise and Mint EO about digestive pains.
Thanks a lot! I have enjoyed this article to the end with growing interest. Now I’m encouraged to update my knowledge on aromatherapy. Best regards from Barcelona (Spain) from a Mexican Pharmacist.
Thanks, Hana, for an excellent article. Are Phyt’Arome proceedings available?
Hi Kath! Thank you for your kind words. I am not sure about the proceedings for Phyt’Arome, and would advise going to the conference’s website for more information on this. Hana
Excellent, thank you for sharing this information.