Personal note: I’ve been working on this article on and off since 2016 when I first came across the concept of smell training as a treatment for smell loss. And while the work has been delayed, at the same time I witnessed the evolution of a clinically approved and endorsed aromatherapy treatment. I hope you’ll join me in discovering the fascinating world of smell disorders and their treatment, and hopefully it won’t take you five years to read the article!
While it may seem that losing your sense of smell is of less consequence than losing vision or hearing, smell loss can have an enormous impact on quality of life. You might have experienced it yourself. Pre-covid statistics suggest that between 4% and 25% of the population suffers from some kind of olfactory disorder ranging from diminished smell capacity (hyposmia) to total loss of smell (anosmia) (Keller and Malaspina, 2013). Many more of us have experience smell loss recently, as it is one of the primary symptoms of Covid-19. The self-reported incidence from surveys varies from 33.9% to 68% of Covid patients. One report states that a whopping 98.6% of covid positive patients had some form of olfactory disorder when assessed clinically, suggesting that incidence may be even higher than the self-reported rates .
Until recently there was no effective treatment, and while for many, olfactory function returns spontaneously within weeks or months, some are left with little to no hope of recovery. But there’s good news! As of January 2021, olfactory training is a recommended treatment for post-infectious olfactory disorder .
But what are olfactory disorders? How can you tell if you have one? How did the research on smell training develop? And what can you do if your sense of smell is impacted, whether by covid or for some other reason?
Olfactory disorders – classification, causes, diagnosis
Olfactory disorder means a distorted sense of smell. Whether it’s heightened, diminished, or whether you’re smelling smells that aren’t really there at all, this means your sense of smell is not functioning as it should. And since it is one of our most primary senses, its impairment can have severe consequences.
There are two principal types of olfactory disorder – quantitative: an altered acuity of our sense of smell; and qualitative: a distorted sense of smell.
The quantitative smell disorders are hyperosmia (overwhelming sensitivity to smells), hyposmia (reduced ability to smell) and anosmia (complete loss of smell). Various olfactory function tests are used for assessment, and you are considered anosmic if your Sniffin Sticks TDI score is below 16.5. This means you are unable to detect virtually any smell, at any intensity. Hyposmia (also referred to as microsmia) is a decreased sense of smell and a Sniffin Sticks score between 16.5 and 30.5 would qualify you as hyposmic. In practical terms this means that your sense of smell is below normal, and you can smell fewer odors, or only odors of higher intensity. In many people, hyposmia develops in older age.
Specific anosmia – or the inability to detect a particular smell or smells – is a sub-category. For example, 8% of the general population cannot smell l-carvone, the primary spearmint odorant (Pelosi and Viti 1978). One study (Croy et al, 2016) showed that if we increase the number of individual tested odor molecules, everyone is likely to be anosmic to at least one of them. In other words, the science suggests that we are all smell-blind to something. For most of us this is of no consequence, since we almost always encounter highly complex odorants containing many specific compounds. So we may all be able to smell coffee, but specific anosmia to one or two of the individual constituents probably means that what each of us perceives may actually differ.
The qualitative disorders, parosmia and phantosmia, are sometimes put under the umbrella name of ‘distorted sense of smell’. Phantosmia means that you perceive a smell that isn’t actually there, while parosmia is a disorder in which a smell is perceived as another, usually very unpleasant smell. This may apply to only certain smells, or all smells. Both parosmia and phantosmia have been linked to Covid-19, may follow on from anosmia or parosmia, and so can occur some weeks after disease onset .
Olfactory disorders are most commonly caused by either a sinonasal infection, commonly viral, or by head trauma. Olfactory disorders can also be congenital (from birth), post-surgical, toxic (from exposure to a toxic substance), or simply unknown, and they can be either acute or chronic conditions. A stuffy nose due to a cold or flu often causes acute hyposmia or anosmia. This may pass or, in rare cases, may become a chronic condition. Covid-19 related anosmia lasts for several weeks to months, so it can be acute, chronic, or subacute – somewhere between the two.
Testing olfactory function
 There are several testing kits available for assessment of olfactory disorders. Most commonly cited are the Sniffin’ Sticks test, devised by Thomas Hummel, the Sniff Magnitude Test, and the Smell Identification Test (UPSIT). More recently, the simplified Le Nez du Vin wine tasting learning kit has also been used. The tested areas are usually detection threshold: how strong does a smell need to be for you to pick it up – and determination: naming different smells. Even with these tests available, many olfactory disorders remain undiagnosed, which is why the prevalence numbers (4-25%) vary so greatly. Many studies on olfactory dysfunction prevalence rely on self-reporting rather than supervised testing. Any of these kits can be purchased online to be self-administered.
There are several testing kits available for assessment of olfactory disorders. Most commonly cited are the Sniffin’ Sticks test, devised by Thomas Hummel, the Sniff Magnitude Test, and the Smell Identification Test (UPSIT). More recently, the simplified Le Nez du Vin wine tasting learning kit has also been used. The tested areas are usually detection threshold: how strong does a smell need to be for you to pick it up – and determination: naming different smells. Even with these tests available, many olfactory disorders remain undiagnosed, which is why the prevalence numbers (4-25%) vary so greatly. Many studies on olfactory dysfunction prevalence rely on self-reporting rather than supervised testing. Any of these kits can be purchased online to be self-administered.
Olfactory dysfunction as a symptom
Increasingly, the medical community is using smell function as a diagnostic tool to determine whether a person is suffering from another disorder, such as Parkinson’s disease or Alzheimer’s disease (Knudsen et al 2015, Walker et al 2021). Hyposmia is also a common symptom of depression, as well as being a cause (Athanassi et al 2021). Smell loss is listed among the primary symptoms of Covid-19 infection, and is an indication for further testing or self-isolation.
The impact of olfactory disorders on quality of life
The ways in which loss or distortion of smell impacts a person’s life may be less obvious than for other sensory impairments, yet they are no less significant. A patient report series called Hidden Consequences of Olfactory Dysfunction (Keller and Malaspina 2013) lists all the ways in which a person with a smell disorder can be disadvantaged. From a practical point of view, olfactory loss limits our ability to avoid hazards such as fire, a gas leak, or food that has gone bad. There is also the inability to enjoy eating, as the odor of a meal contributes significantly to the experience, resulting in loss of appetite in some, and weight gain in others.
Personal hygiene can be affected, too. “For those who lost their sense of smell, odor management is also difficult. Without a sense of smell it is impossible to verify that one’s body, children, or home do smell acceptable” (Keller and Malaspina 2013). The consequences of this handicap can translate to children either sitting in dirty diapers for too long, or being compulsively changed too often. Paranoia about one’s own body odor can easily lead to social isolation, fear of intimacy, and withdrawal. Combine all of the above with feelings of loss and frustration, and it is no surprise that patients with olfactory disorders almost always experience decreased quality of life.
And while suffering from depression can come with hyposmia, loss of smell can also induce depression. As with any other sense, losing our smell decreases our general enjoyment of life – just think about all the food smells, nature smells and perfumes you encounter and love on a daily basis, and then imagine the world without them.
A gym for your nose – the evolution of olfactory training
The idea that we can train our nose to recognize an odor that we had lost the ability to detect came from a 1980s research study on androstenone. This is a mammalian pheromone that about 50% of people cannot smell. Charles Wysocki, an olfaction researcher, was one of those people, until he was exposed to the substance for several months as part of his work. Seeing his specific anosmia reversed, he then conducted further research with volunteers, showing exactly what he experienced – that repeated exposure to a specific odorant can train our nose to recognize it.
 Some years later, Thomas Hummel of the Smell and Taste Clinic at Dresden University in Germany decided to take the idea further. He wanted to find out if he could help his patients with olfactory disorders. He devised a protocol for olfactory training in hyposmic or anosmic patients, which has since been tested in many clinical studies. In 2009, Hummel and colleagues published a study entitled Effects of Olfactory Training in Patients with Olfactory Loss. This was a prospective study on 56 people with some form of olfactory dysfunction, and it established the standard procedure for olfactory training.
Some years later, Thomas Hummel of the Smell and Taste Clinic at Dresden University in Germany decided to take the idea further. He wanted to find out if he could help his patients with olfactory disorders. He devised a protocol for olfactory training in hyposmic or anosmic patients, which has since been tested in many clinical studies. In 2009, Hummel and colleagues published a study entitled Effects of Olfactory Training in Patients with Olfactory Loss. This was a prospective study on 56 people with some form of olfactory dysfunction, and it established the standard procedure for olfactory training.
The protocol consists of systematic exposure to four odorant substances over a period of 12 weeks. These were selected based on the ‘odor prism’ theory established by Henning in 1916 and representing four of the six categories in that theory: flowery, fruity, resinous and aromatic. The odorants used are undiluted single chemicals: phenylethanol (rosy), 1,8-cineole (eucalyptus), citronellal (lemony) and eugenol (clove). In olfactory training, each odor is smelled for just ten seconds each morning and evening. As we will see later, some researchers got inventive with their array of odors, though none seem to have used whole essential oils.
Does smell training work?
The research shows that, with some limitations, it does. The original 2009 study saw a significant improvement in the olfactory training group compared to the control group, and the improvement was seen in people with anosmia resulting from different causes (Hummel et al 2009). Subsequent studies have confirmed this finding, and tried modifying the protocol (training for longer, with different odorants, at different intensities). Here are some highlights of the research:
- A 2012 study researched the impact of an 8-month period of olfactory training in patients with olfactory dysfunction (Fleiner et al 2012). They studied 46 patients with olfactory dysfunction with different etiologies – post-infectious, post-traumatic and idiopathic. After four months of exposure to four odorants twice daily, olfactory function increased significantly for the post-infection olfactory dysfunction patients. This group saw the most significant increase, however there was no further improvement after the four month period. Unfortunately the researchers found that those who had suffered from an olfactory disorder for longer than two years before olfactory training did not see any improvement. This study used more varied odors for their training: rose, orange, citrus, peppermint, raspberry, chocolate, vanilla, cinnamon and leather. These were fragrance oils, not essential oils. Four months seems to be the sweet spot, and it also needs to be said that the sooner you start with the training, the better.
- Some researchers experimented with the protocol – one study examined whether the use of more than four odors, plus an extension of the training period, might lead to better results (Altundag et al, 2015). The 85 subjects of this study were divided into three groups – one performed olfactory training twice daily for 36 weeks with the standard four odors. The second group switched odors every 12 weeks. They started with phenylethanol, 1,8-cineole, citronellal, eugenol; first switch to menthol, thyme, tangerine, jasmine; last group of odors was green tea, bergamot, rosemary, gardenia. (It’s not clear whether any of these were essential oils.) The third group was a control. Although two other studies (Hummel et al, 2009 and Damm et al, 2014) examined olfactory training for 12 and 18 weeks respectively with no significant difference, this study found a continuous improvement from baseline to the end of the observation period. However, the improvement slowed significantly after 24 weeks. The three groups reached similar threshold scores, but the determination capabilities of the group that rotated odors were significantly higher – switching the odors around was indeed beneficial. All the subjects in this study suffered form an olfactory disorder that followed a respiratory tract infection.
- An even more robust randomized, controlled, multicenter study involving 144 patients focused on the efficacy of OT for post-infectious anosmia (Damm et al 2014). Participants were divided into two groups: one group performed a high-intensity OT for 18 weeks, and then switched to low intensity OT for another 18 weeks, the other group did OT in reverse order (low-high). Olfactory training consisted of sniffing twice daily felt-tip pens with the four standard odorants: phenylethanol, 1,8-cineole, citronellal, eugenol. In the low intensity training, 0.0001% concentrations were used. This was determined to be the lowest detectable threshold concentration for a healthy population. The high-intensity group used undiluted odorants. In the high-intensity group, 25% of participants showed improved olfactory function, compared to 15% in the low intensity group after the initial 18 weeks of training. After the completion of the full 36 weeks, a total of 30.8% participants in the low-high group experienced improved olfactory function, compared to 45.8% in the high-low group. In the groups combined, the number of participants with anosmia more than halved (36.3% to 15.3%) and 8.9% of participants became normosmic. The best results were obtained where anosmia had lasted for less than 12 months.
There are some limitations to available studies on olfactory training. None of the ones mentioned here or reviewed elsewhere used a control group that would sniff blank carriers, which would help establish whether it’s the odor or just the act of active and conscious sniffing that has an effect. The selection of odors is either based on an outdated odor classification system (the prism), or not justified. The length of the protocol also varies across studies. No studies appear to have used whole essential oils – they were either single chemicals, or fragrance oils. It would be interesting to compare the results of using essential oils for added therapeutic benefits such as anti-inflammatory, neuroprotective and regenerative. However, the results are still very impressive and noteworthy!
How does it work?
So, if we know that olfactory training does work, do we also know how it works? We know that it has to do with the trigeminal nerve, as well as with the neural plasticity of our brains (Sorokowska et al 2016). To put it simply, our brains are capable of creating new neural connections, and bypassing those that no longer function.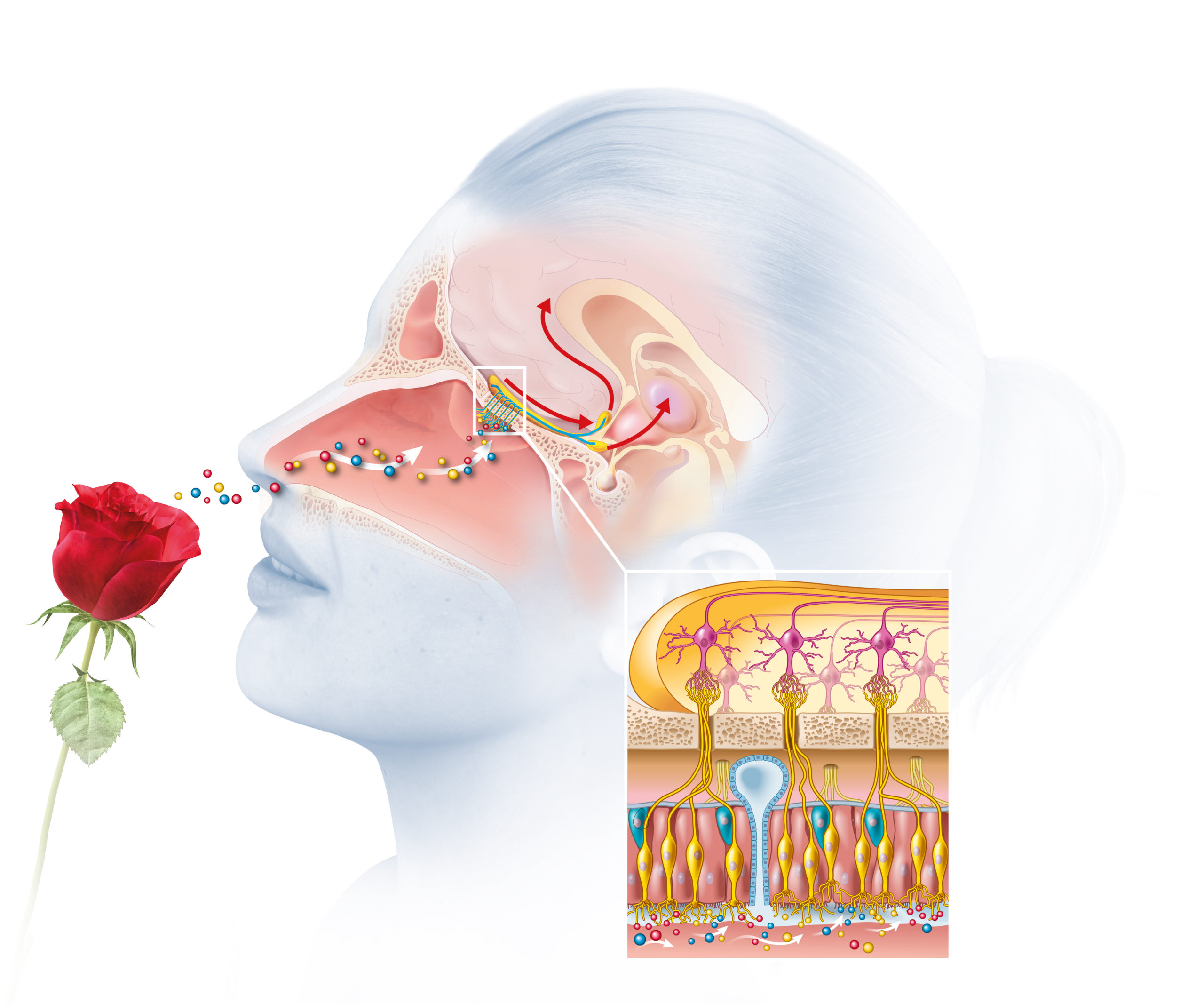
- A study looked at changes in the brain of anosmic patients after 12 weeks of olfactory training (Kollndorefer et al 2015). The patients chose four odors out of six options (cinnamon, vanilla, orange, rose, menthol, banana) and sniffed them twice daily. A functional MRI scan was performed before and after the training. The researchers found new functional connections in the brain after the training, especially in those brain centers that are responsible for olfaction. To put this in more general terms: When our sense of smell has either deteriorated or is completely non-functional, the connections in our brain that enable us to process smell sensations correctly are disrupted. This study showed that olfactory training helps regenerate those connections at the level of nerve cells.
The trigeminal nerve also plays an important role. This is a peripheral chemosensory nerve, responsible for the perception of noxious substances. When you smell ammonia, for example, the stinging sensation is mediated by your trigeminal nerve. This seems to play an important role in restoring the sense of smell (Doty et al, 1978).
Olfactory training as a clinically endorsed treatment
There is now a solid body of evidence for olfactory training as a treatment for olfactory disorders. At the same time, the incredible increase in patients suffering decreased sense of smell due to the Covid-19 pandemic created an acute need for a solution. It is no surprise then that the intervention has been endorsed and recommended by clinicians, most recently by a Clinical Olfactory Working Group in May 2021. Interestingly, the protocol endorsed in the Working Group consensus uses whole essential oils.
While the protocols vary from 12 to 56 weeks (with 16 weeks seemingly the sweet spot for improvement, see Konstantinidis et al 2016), all the research shows that optimum results are obtained for those who suffer hyposmia or anosmia as a result of an upper respiratory tract infection, and the greatest improvement is seen within 12 months from the onset of olfactory dysfunction.
The standard protocol, as mentioned by this publication is sniffing of the four odorants (1,8-cineole, eugenol, phenylethanol, citronellal) twice daily for 20 seconds each (longer than Hummel’s original protocol), and for at least 24 weeks. That’s six months, so it does require a lot of patience and discipline. This is not a quick fix, and it should be approached more as a way to slowly rehabilitate your sense of smell, like you would retrain yourself to walk after knee surgery, for example.
Can you train at home?
 Are you suffering from anosmia and you’d like to try the intervention, or would you like to see if you can improve your sense of smell? There are many resources available to guide you through the process.
Are you suffering from anosmia and you’d like to try the intervention, or would you like to see if you can improve your sense of smell? There are many resources available to guide you through the process.
First, I would recommend taking an objective smell test – either through an ORL specialist, or self-administered. You can order three of the tests mentioned for home use (Sniffin’ Sticks, UPSIT and Le Nez du Vin). Once you have your baseline noted, you can then start training. Knowing your baseline is important because it will help you measure your progress objectively.
Then you can look for one of these resources for olfactory training:
https://www.fifthsense.org.uk/smell-training/ (protocol recommended by Clinical Olfactory Working group, also additional materials such a training journals)
https://abscent.org/learn-us/smell-training
The Smell Gym by Frauke Galia
All of these use essential oils in their training protocols, so you don’t have to try and find single chemicals.
The question is whether you need to be using the specific odors – Rose, Eucalyptus, Clove and Lemon – and the research to date suggests that it may not be as much about what you are smelling, as it is about really doing it consistently for a long period of time.
Anosmia and aromatherapy
In aromatherapy circles, a question sometimes arises about whether essential oils can help people who have no sense of smell. Mostly these questions relate to other health conditions – and while an anosmic person cannot enjoy the complex aroma of an essential oil, they can most certainly benefit from their biological actions, such as soothing inflammation or alleviating pain.
But now we also know that olfactory training with the use of essential oils can help with the loss of smell itself, which is incredible news. This is, after all, true aroma – therapy!
In conclusion
It is not very often that we see the development of a clinically endorsed aromatherapy-based protocol in real time, but that is what has happened with olfactory training as a treatment for smell disorders, whether it’s anosmia or hyposmia. This brings great hope to the millions of people who have been impacted by partial or total smell loss. It is also a great opportunity for those who work with essential oils to assert their place in the healthcare landscape.
Olfactory training can be used in post-infectious rehabilitation, but it also shows some promise for patients with cognitive dysfunction (dementia) and even psychological issues.
Citations:
Addison, Alfred B., Billy Wong, Tanzime Ahmed, Alberto Macchi, Iordanis Konstantinidis, Caroline Huart, Johannes Frasnelli, et al. “Clinical Olfactory Working Group Consensus Statement on the Treatment of Postinfectious Olfactory Dysfunction.” The Journal of Allergy and Clinical Immunology 147, no. 5 (May 2021): 1704–19. https://doi.org/10.1016/j.jaci.2020.12.641.
Altundag, Aytug, Melih Cayonu, Gurkan Kayabasoglu, Murat Salihoglu, Hakan Tekeli, Omer Saglam, and Thomas Hummel. “Modified Olfactory Training in Patients with Postinfectious Olfactory Loss: Treatment of Olfactory Loss.” The Laryngoscope 125, no. 8 (August 2015): 1763–66. https://doi.org/10.1002/lary.25245.
Athanassi, Anna, Romane Dorado Doncel, Kevin G Bath, and Nathalie Mandairon. “Relationship between Depression and Olfactory Sensory Function: A Review.” Chemical Senses 46 (January 1, 2021): bjab044. https://doi.org/10.1093/chemse/bjab044.
Croy, I., S. Nordin, and T. Hummel. “Olfactory Disorders and Quality of Life–An Updated Review.” Chemical Senses 39, no. 3 (March 1, 2014): 185–94. https://doi.org/10.1093/chemse/bjt072.
Croy, I., S. Olgun, L. Mueller, A. Schmidt, M. Muench, G. Gisselmann, H. Hatt, and T. Hummel. “Spezifische Anosmie als Prinzip olfaktorischer Wahrnehmung.” HNO 64, no. 5 (May 2016): 292–95. https://doi.org/10.1007/s00106-016-0119-9.
Damm, Michael, Louisa K. Pikart, Heike Reimann, Silke Burkert, Önder Göktas, Boris Haxel, Sabine Frey, et al. “Olfactory Training Is Helpful in Postinfectious Olfactory Loss: A Randomized, Controlled, Multicenter Study: Olfactory Training.” The Laryngoscope 124, no. 4 (April 2014): 826–31. https://doi.org/10.1002/lary.24340.
Fleiner, Franca, Larissa Lau, and Önder Göktas. “Active Olfactory Training for the Treatment of Smelling Disorders.” Ear, Nose, & Throat Journal 91, no. 5 (May 2012): 198–203, 215. https://doi.org/10.1177/014556131209100508.
Henning, Hans. Der Geruch. Leipzig: Barth, 1916.
Hummel, Thomas, Karo Rissom, Jens Reden, Aantje Hähner, Mark Weidenbecher, and Karl-Bernd Hüttenbrink. “Effects of Olfactory Training in Patients with Olfactory Loss.” The Laryngoscope 119, no. 3 (March 2009): 496–99. https://doi.org/10.1002/lary.20101.
Keller, Andreas, and Dolores Malaspina. “Hidden Consequences of Olfactory Dysfunction: A Patient Report Series.” BMC Ear, Nose and Throat Disorders 13, no. 1 (December 2013): 8. https://doi.org/10.1186/1472-6815-13-8.
Knudsen, K., M. Flensborg Damholdt, K. Mouridsen, and P. Borghammer. “Olfactory Function in Parkinson’s Disease – Effects of Training.” Acta Neurologica Scandinavica 132, no. 6 (December 2015): 395–400. https://doi.org/10.1111/ane.12406.
Kollndorfer, K., F.Ph.S. Fischmeister, K. Kowalczyk, E. Hoche, C.A. Mueller, S. Trattnig, and V. Schöpf. “Olfactory Training Induces Changes in Regional Functional Connectivity in Patients with Long-Term Smell Loss.” NeuroImage: Clinical 9 (2015): 401–10. https://doi.org/10.1016/j.nicl.2015.09.004.
Konstantinidis, I., E. Tsakiropoulou, and J. Constantinidis. “Long Term Effects of Olfactory Training in Patients with Post-Infectious Olfactory Loss.” Rhinology Journal 54, no. 2 (June 1, 2016): 170–75. https://doi.org/10.4193/Rhino15.264.
Kronenbuerger, Martin, and Manfred Pilgramm. “Olfactory Training.” In StatPearls. Treasure Island (FL): StatPearls Publishing, 2021. http://www.ncbi.nlm.nih.gov/books/NBK567741/.
Meng, Xiangming, Yanzhong Deng, Zhiyong Dai, and Zhisheng Meng. “COVID-19 and Anosmia: A Review Based on up-to-Date Knowledge.” American Journal of Otolaryngology 41, no. 5 (September 2020): 102581. https://doi.org/10.1016/j.amjoto.2020.102581.
Pekala, Kelly, Rakesh K. Chandra, and Justin H. Turner. “Efficacy of Olfactory Training in Patients with Olfactory Loss: A Systematic Review and Meta-Analysis: Systematic Review of Olfactory Training.” International Forum of Allergy & Rhinology 6, no. 3 (March 2016): 299–307. https://doi.org/10.1002/alr.21669.
Pelosi, Paolo, and Raffaella Viti. “Specific Anosmia to l -Carvone: The Minty Primary Odour.” Chemical Senses 3, no. 3 (1978): 331–37. https://doi.org/10.1093/chemse/3.3.331.
Rumeau, C., D.T. Nguyen, and R. Jankowski. “How to Assess Olfactory Performance with the Sniffin’ Sticks Test ®.” European Annals of Otorhinolaryngology, Head and Neck Diseases 133, no. 3 (June 2016): 203–6. https://doi.org/10.1016/j.anorl.2015.08.004.
Schambeck, Sophia E., Claudia S. Crowell, Karolin I. Wagner, Elvira D’Ippolito, Teresa Burrell, Hrvoje Mijočević, Ulrike Protzer, et al. “Phantosmia, Parosmia, and Dysgeusia Are Prolonged and Late-Onset Symptoms of COVID-19.” Journal of Clinical Medicine 10, no. 22 (November 12, 2021): 5266. https://doi.org/10.3390/jcm10225266.
Sorokowska, A., E. Drechsler, M. Karwowski, and T. Hummel. “Effects of Olfactory Training: A Meta-Analysis.” Rhinology 55, no. 1 (March 1, 2017): 17–26. https://doi.org/10.4193/Rhin16.195.
Walker, Ian M., Michelle E. Fullard, James F. Morley, and John E. Duda. “Olfaction as an Early Marker of Parkinson’s Disease and Alzheimer’s Disease.” Handbook of Clinical Neurology 182 (2021): 317–29. https://doi.org/10.1016/B978-0-12-819973-2.00030-7.


Very timely and well researched article, Hana.
An additional benefit to The olfactory training would be the firing of new neural pathways in the brian that would reduce memory loss (and alzheimers) in participants.
Thank you for posting this what a great article. I suffered with it a little before covid 19 and it just got worse after I contracted covid 19 which I have long term covid now because of my immune system issues.
Can’t wait to try and see the results. I’m also thinking that maybe in doing so so I could help with some of the immune and pain issues that I do have in the process Since the old factory system really sets off a lot of great things. We shall see. If it does I would love to help others with this. Thanks again
Thank you very much, very interesting and useful!
que matéria fantástica!!! suas informações são riquíssimas, obrigada!
this article was fascinating in that this training can form new neural pathways in our brain thru the nerve mentioned. my mother suffers from low sense of smell due to working around cosmetology chemicals. we will definitely research the “at home” training, perform our own testing and see what results. thank you hana for such an in-depth look into the olfactory system!