by Sue Pace
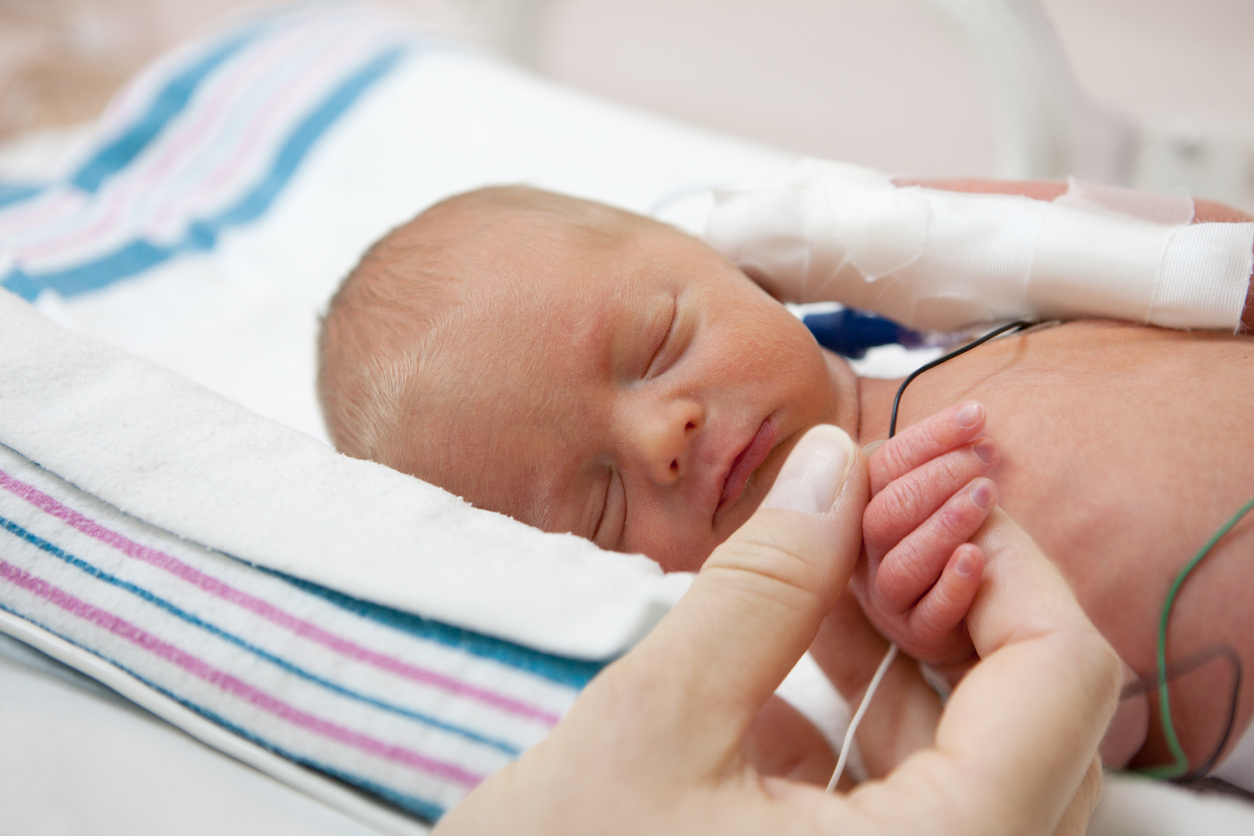
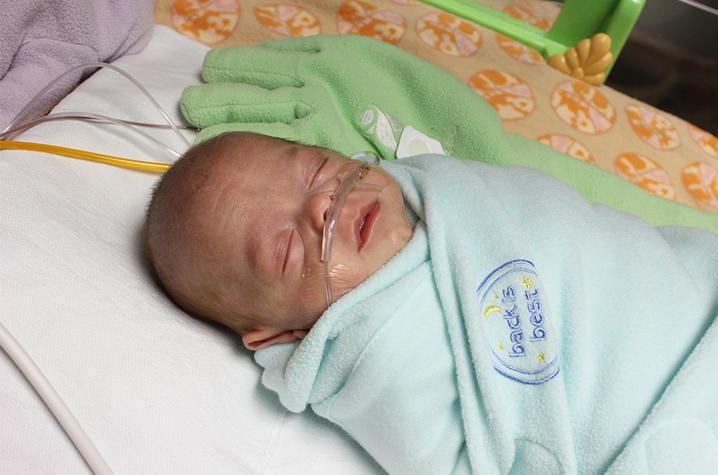
A newborn baby girl lies swaddled in a receiving blanket in her isolette. While she has ten fingers and ten toes, rosebud lips, and a great shock of dark hair, this baby somehow doesn’t look or act ’right’. Weighing only 6 lbs (2722 g) at birth, her muscles tremble and twitch whenever she turns her head towards lights, hears a noise, or is picked up for a diaper change. She frequently vomits her formula, cries unceasingly from morning until night, and she’s even had a seizure. The reason for these symptoms: the baby girl’s mother had opiates in her system when she was born.
Neonatal abstinence syndrome (NAS), sometimes referred to as neonatal withdrawal syndrome, is defined as “a group of problems that occur in a newborn who was exposed to addictive opiate drugs while in the mother’s womb” . Once the umbilical cord, the lifeline and connection between mother and child is severed, babies begin life as separate human beings. No longer exposed to opiates in the mother’s system, babies start experiencing narcotic withdrawal . While opiates cause some of the worst withdrawal signs seen in NAS, they are not the only class of drugs responsible for producing symptoms. Medications in the benzodiazepine class (Ativan, Xanax, etc.) and less commonly antidepressants or barbiturates can also cause withdrawal symptoms in newborns .
When mothers of these infants come to mind, a mental picture may form of a pregnant, desperate heroin junkie ‘shooting up’ in a back alley somewhere. While this undoubtedly occurs, far more pregnant women abuse prescription opiate pills than use IV drugs. Also, there are pregnant women on a substitution regimen of oral/sublingual medications like methadone or buprenorphine which are part of a maintenance plan designed to help keep them free from intravenous drug use .
The severity of symptoms seen in babies born with NAS depends on several factors :
- The drug the mother is taking
- How often the drug is taken
- The dose that is taken
- The time of the last drug exposure before birth
- The mother’s rate of metabolizing the drug
Many NAS babies will need narcotic medication, chiefly morphine, to help them cope with withdrawal from maternal opiate use, while some protocols call for the use of oral methadone or sublingual buprenorphine as narcotic replacements. Hospital stays can vary dependent on the type of drug the mother was taking. Shorter-acting medications like Vicodin, which has a plasma elimination half-life of approximately four hours, may result in briefer hospital stays for affected babies than drugs with a longer half-life such as methadone (plasma elimination half life of 8-59 hours) . The costs associated with neonatal abstinence syndrome are staggering. NICU charges can range from $3,000-6,000 per day and NAS babies have hospital stays ranging from 17-23 days while undergoing pharmacologic intervention . Since many women who abuse opiates are underinsured, the burden of costs to the hospital are back-breaking as well. Affected babies can take weeks or months to finally wean off a cocktail of medications.
Aromatherapy study
Lori Shook, M.D., is a University of Kentucky neonatologist and horse owner who has significant experience with NAS babies. Dr. Shook had seen first-hand the calming effect of lavender essential oil while working with skittish horses. She and pediatric fellow John Daniel, M.D. wondered if essential oils could act as an adjunct therapy to help reduce agitation in their tiny patients. Aware that complementary therapies are often viewed with suspicion by the traditional medical community, Dr. Daniel stated “There is a lot of complementary alternative medicine research out there that is not subjected to rigorous scientific methodology…. when we started this project, that was our goal” .
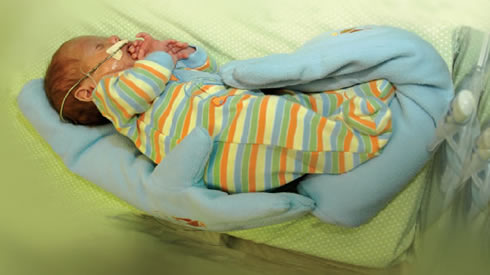
In 2015, the two physicians began a pilot study enrolling infants with NAS in a randomized controlled trial scheduled to conclude in July 2017. The study examines the use of an aromatherapy patch impregnated with lavender (Lavandula angustifolia) and Roman chamomile (Chamaemelum nobile) essential oils placed on a fabric bolster surrounding the baby . Called a ‘Zaky arm’, the bolster is designed to “simulate the shape, warmth, weight…and touch of the parents’ hands and forearms”
As the aromatherapy patches were not previously classified by the U.S. Food and Drug Administration as drugs/medication, an investigational new drug application (NDA) was filed with the agency, which subsequently approved it for the purposes of the trial .
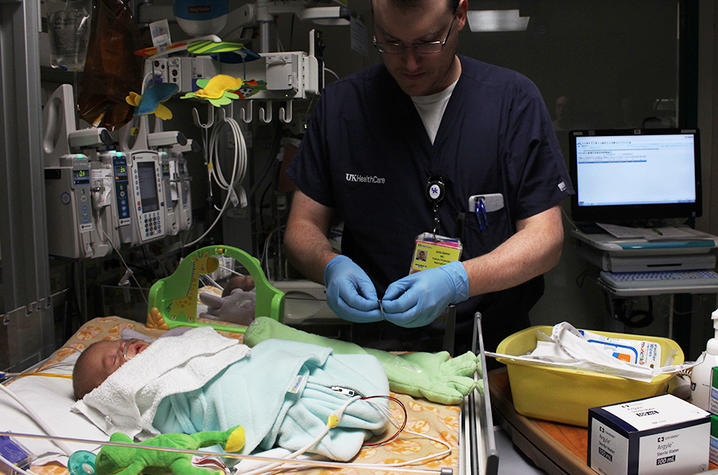
Outcomes of the study are designed to measure the length of hospitalization and the time elapsed before traditional medications are employed. The treatment group of infants receives an aromatherapy patch on the Zaky arm plus standard care, which includes morphine replacement therapy, infant massage, and physical, occupational, and music therapy. The control group receives standard care but without aromatherapy .
Although the study has been ongoing, preliminary results show demonstrable positive effects. Babies in the aromatherapy treatment group shortened their NICU stay by an average of 6.4 days as compared to infants not receiving the aromatherapy treatment. In addition, babies receiving aromatherapy required smaller doses of traditional medications than infants who had only standard care. This has resulted in significant cost savings to the hospital .
Mark Theno, CEO and developer of the Bioesse™ aromatherapy patch, worked with the University of Kentucky NICU team and says he’s received much positive feedback from staff employing the patches during the study. He stated “not only did they enjoy using the patches with their tiny patients, they were so impressed with the preliminary results that they’re considering doing a patch study to track effects on staff stress/sleep patterns” .
In certain carefully selected instances, the use of aromatherapy may help infants (and their families) adversely affected by maternal narcotic use. By shortening NICU stays and reducing staff stress, hospitals also reap the benefits of this healing intervention. This study builds on previous work showing low-level odors can be used therapeutically in newborns .
This is a study that uses minimal ambient diffusion of essential oils. Note that most professional aromatherapists agree that applying even highly diluted essential oils to newborn skin is best avoided. The immaturity and fragility of newborn skin makes it more sensitive to insult than the skin of older infants and children .
References
- Neonatal Abstinence Syndrome. Retrieved from MedLine Plus Medical Encyclopedia, https://medlineplus.gov/ency/article/007313.htm, June 10, 2017
- McQueen, K., Murphy-Oikonene, J. (2016). Neonatal abstinence syndrome. New England Journal of Medicine, 375(25), 2468-2479. http://www.nejm.org/doi/pdf/10.1056/NEJMra1600879
- “Neonatal Abstinence Syndrome.” Retrieved from Medscape website, http://emedicine.medscape.com/article/978763-overview#a5, June 10, 2017.
- “Vicodin (hydrocodone bitartrate and acetaminophen) tablets”. Retrieved from RxList website, www.rxlist.com/vicodin-drug.htm, July 18, 2017.
- “Dolophine (methadone) tablets.” Retrieved from RxList website, www.rx.list.com/dolophine-drug.htm, July 18, 2017.
- “Dramatic Increases in Maternal Opioid Use and Neonatal Abstinence Syndrome”. Retrieved from the National Institutes on Drug Abuse website, https://www.drugabuse.gov/related-topics/trends-statistics/infographics/dramatic-increases-in-maternal-opioid-use-neonatal-abstinence-syndrome, June 10, 2017.
- “Total costs of treatment for babies with neonatal abstinence syndrome on the rise”. Retrieved from the News-Medical.net website, http://www.news-medical.net/20150520/Total-costs-of-treatment-for-babies-with-neonatal-abstinence-syndrome-on-the-rise.aspx. June 10, 2017.
- Lee, J., Hulman, S., Musci, M., et al (2015). Neonatal abstinence syndrome: Influence of a combined inpatient/outpatient methadone treatment regimen on the average length of stay of a medicaid NICU population. Population Health Management, 18(5), 392-397. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4675180/pdf/pop.2014.0134.pdf
- Adams, E. (2017). Pediatric experts find aromatherapy effective for promoting infant healing, nas recovery. Retrieved from the University of Kentucky News website, https://uknow.uky.edu/uk-healthcare/pediatric-experts-find-aromatherapy-effective-promoting-infant-healing-nas-recovery, June 10, 2017.
- Daniel, J. (2017). The effect of aromatherapy on neonatal abstinence syndrome and salivary cortisol levels. Retrieved from the ClinicalTrials.gov website, https://clinicaltrials.gov/ct2/show/NCT03097484, June 10, 2017.
- “What are the Zakys, use, NICU process standard, comparison.” Nurtured by Design website, http://www.nurturedbydesign.com/en/thezaky/medical-staff_thatis-uses.php, June 10, 2017.
- Theno, M. (2015). Can aromatherapy help neonatal babies get through opioid withdrawal? Cision PR Newswire, https:// prnewswire.com/news-releases/can-aromatherapy-help-neonatal-babies-get-through-opioid-withdrawal-300181585.html, June 30, 2017.
- Tisserand, R., Young, R. (2014). Essential oil safety, 2nd edition. Churchill Livingstone, Edinburgh, p 97.
- Edraki, M., Pourpulad, H., Kargar, M. et al (2013). Olfactory stimulation by vanillin prevents apnea in premature newborn infants. Iranian Journal of Pediatrics, 23(3), 261–268. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3684469/
- Goubet, N., Strasbaugh, K., Chesney, J. (2007). Familiarity breeds content? Soothing effect of a familiar odor on full-term newborns. Journal of Developmental and Behavioral Pediatrics, 28(3), 189–194. http://doi.org/10.1097/dbp.0b013e31802d0b8d
- Kawakami, K., Takai-Kawakami, K., Okazaki, Y. et al (1997). The effect of odors on human newborn infants under stress. Infant Behavior and Development, 20(4), 531–535. http://doi.org/10.1016/S0163-6383(97)90041-2
- Marlier, L., Gaugler, C., Messer, J. (2005). Olfactory stimulation prevents apnea in premature newborns. Pediatrics, 115, 83–88. http://doi.org/10.1542/peds.2004-0865

This sounds fascinating where can I get a copy of the trial detailing the methodology used? The zacky arm looks in itself a soothing factor. Many thanks
Hi Fran, in the article’s references, number10 lists the clinical trial and its methodology.
Link: https://clinicaltrials.gov/ct2/show/NCT03097484